What is skin cancer?
Skin cancer is the out-of-control growth of abnormal cells in the outermost skin layer, the epidermis. These cells grow more quickly and don’t make skin normally. This results in lumps, scaling, ulcers and bleeding. The main types of skin cancer are basal cell carcinoma (BCC, often called a rodent ulcer), squamous cell carcinoma (SCC) and melanoma.
What causes skin cancer?
Ultraviolet light, either from the sun or sunbeds, is the best known cause of skin cancer. This light is absorbed by skin cells and damages their DNA. This causes mutations leading to uncontrolled cell growth. As a result, skin cancer is seen more often on sun exposed skin, in people with paler skin and in sunnier climates.
Despite the strong link with sun exposure many cases of skin cancer have no clear cause.

What are the early signs of skin cancer?
The good news is that if it is caught early, there is a good chance that skin cancer can be treated with little scarring and complete elimination. Often, the doctor can detect the growth at a precancerous stage, before it has penetrated beneath the surface of the skin or become fully malignant. At this stage the skin might look red and flaky, start to thicken or even develop hard patches. To diagnose these areas a biopsy (sample) under local anaesthetic might be needed. This can help guide whether to treat with full removal or with freezing or creams.
Types of Skin Cancer
The 3 commonest types of skin cancer are basal cell carcinoma, squamous cell carcinoma and melanoma.
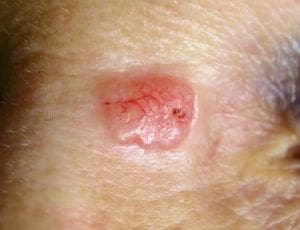
Basal Cell Carcinoma (BCC, rodent ulcer)
This is the commonest type of skin cancer and arises from the deeper ‘basal’ cells of the outer skin layer, the epidermis. Basal cell carcinoma (BCC) is linked to sun or ultraviolet light exposure and is commonest on sun exposed areas, especially the face, ears, scalp, neck, shoulders and back. BCC commonly looks like a shiny lump or red patch, sometimes with small blood vessels, or as an ulcer with a raised, rolled edge. Less commonly it appears as an open sore or scar. If a BCC is left for a long time it can grow and seem to be eating away its surroundings. This was thought to look like a rat bite, giving BCC its nickname of ‘rodent ulcer’. It is very rare for BCCs to spread.
BCCs are most commonly treated with surgery to completely remove them. Because they can be larger than is visible with the naked eye, to achieve this your surgeon will take a safety margin of up to 5mm of normal skin. This will completely remove 19 out of 20 (95%). If a BCC is not completely removed then further surgery is usually advisable.
The size and site of a BCC will determine the scarring after surgery. Sometimes a skin graft or flap is needed. A Plastic Surgeon is trained to give the best appearance possible.
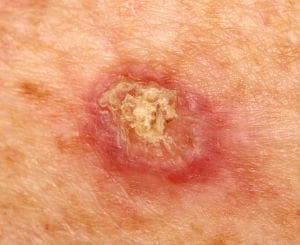
Squamous Cell Carcinoma (SCC)
SCC is the second commonest type of skin cancer. It arises from the outer cells of the epidermis that normally shed continuously as dry skin. As a result, SCCs often have a scaly appearance or a hard covering called keratosis, usually on top of a pink lump. Their growth sometimes outstrips this covering making a raw, ulcerated surface. Because of this, SCCs can sometimes crust, itch or bleed.
SCCs are most common on sun exposed skin, including the face, lips, ears, scalp and hands. They are also sometimes found in long standing wounds.
SCCs don’t often spread and if they do, it’s most commonly to the deeper layers of the skin. They can spread to nearby lymph nodes and around the body, but this is unusual.
The treatment of SCCs often involves a biopsy to confirm the diagnosis and whether there is a low or high risk of spread. This biopsy might remove the whole SCC if it is small. If the SCC is large or high risk then a second operation might be needed, sometimes with a skin graft or flap.
After an SCC you should protect your skin from the sun and check it regularly for any sign of regrowth or new SCCs, even after complete removal, as there is a low chance of the cancer returning. For SCCs with a high risk of spread your doctor may advise regular checkups.
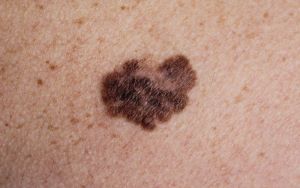
Melanoma
Melanoma is a cancer that develops from melanocytes, the pigment cells that give skin it’s brown colour. Like other types of skin cancer it is linked to ultraviolet rays from the sun or sunbeds. These rays create a tan by stimulating melanocytes to make pigment but can also damage DNA resulting in uncontrolled cell growth and cancer. Melanoma is often triggered by the intense, intermittent sort of sun or sunbed exposure that can cause sunburn, and can appear many years afterwards.
Melanomas often closely resemble moles and can arise from them. However, they are usually less evenly shaped, have irregular surfaces and colours and can grow. They can also ulcerate and cause symptoms including bleeding, leaking, pain and itch.
Melanoma is the most serious of the 3 common types of skin cancer. If it is caught and treated early it can be curable. When melanoma has spread deeper into the skin or other parts of the body, it becomes harder to treat and can be deadly.
The treatment of melanoma involves an initial biopsy to remove the suspicious area with a 2 mm safety margin, confirm the diagnosis and determine the thickness. A melanoma’s thickness is an indication of how likely it is to spread to the surrounding area. More of this area, 1 or 2 cm depending on thickness, is then removed at a second operation, taking all the tissue down to the muscle coverings. A skin graft or flap may be required.
Tests and follow up may be needed. Your doctor will examine the closest lymph glands. Depending on thickness of the melanoma other tests like sentinel lymph node biopsy or CT scanning may be needed. For invasive melanoma your doctor will follow you up regularly for up to 5 years.